THE FINAL SAY
January 13, 2025
 Of the 1048 Brighter Smiles columns published over the last 19 years, I will admit, I repeated a few. Trying to think of new things to write about, other than the importance of an electric toothbrush, water pik, and consistent professional care was challenging after a while. Sometimes I would re-write them completely, and other times I would just tweak them. I would often change the title, depending on how I changed the content.
Of the 1048 Brighter Smiles columns published over the last 19 years, I will admit, I repeated a few. Trying to think of new things to write about, other than the importance of an electric toothbrush, water pik, and consistent professional care was challenging after a while. Sometimes I would re-write them completely, and other times I would just tweak them. I would often change the title, depending on how I changed the content.
One of my favorite columns, which was repeated a few times over the years, always went by the same title; 5 Reasons People Avoid the Dentist. There are no valid reasons not to avoid seeing a dentist on a regular schedule.
Those 5 reasons people avoid the dentist are money, time, lack of concern, fear and trust. The first 3 are excuses. The other 2 can certainly be stumbling blocks for some people; however, they are fixable.
You would think that money would be the biggest reason people avoid the dentist. It isn’t. While some dentistry may be costly, most problems are preventable with long-term consistent professional maintenance care. For the average person without dental insurance, that would cost less than a cell phone plan. Good health always requires awareness, acknowledgement, and investment. While we could argue the role that dental insurance plays, the fact of the matter is, – it’s your health and your choice.
Time is an excuse, period. Lack of concern about dental health is the most common reason people avoid the dentist. Absence of pain is not a good indicator of health. You certainly have the right to not care about your health, but if you do, take care of the gateway to the rest of your body.
I’m not going to comment much on fear today. There should be a minimal amount of fear with today’s dentistry. If you do have fear, you’ll also have to overcome the last reason people avoid the dentist, which is trust. There are many reasons why some patients have a lack of trust in providers. The provider-patient relationship should be based on mutual respect and trust. Continuity of care with as few different providers as possible over your lifetime, is in the patient’s best interest.
Another one of my favorite columns was The Most Important Gift.
As with many aspects of life, people often seem “pre-programmed” about what to expect in a dental office. I, and most of the dentists I know in this area, believe the philosophy of practice revolves around treating the person as a whole, and not just a tooth. It means patients, their overall health & well-being, must be foremost in the practitioner’s mind. Yes, it also means cleanings, fillings and crowns. These are often inescapable outcomes to dental disease – but, under what context are these services being provided?
It didn’t take me too many years to figure out that you can’t treat everyone the same. There are those patients who need every last detail explained, and there are those who don’t want to hear anything, and/or won’t do anything you tell them.
There are dental offices that just view the patient as a mouth of teeth. The goal is to fix as many problems in as many mouths in as short a time as possible. The patient becomes the object of the “fix”, instead of a participant in the treatment. How degrading is it for a patient to experience that type of environment? Where is the quality, attention and care when the dentist is busy running room to room? There may be patients who prefer that environment, so there is something for everyone.
In a truly health-centered practice, each patient should be treated as a unique, whole person. Each patient should be treated with dignity and respect. The dentist gives each patient his/her most important gift: TIME.
The best care involves taking the time to listen, taking the time to do a complete examination, taking the time to teach the causes of existing and potential dental problems, and taking the time to explain alternative treatments and modes of prevention. It means that each patient be given the opportunity to choose the highest level of health consistent with their values and life circumstances.
I appreciate the many people who have given me feedback from reading this column over the years. I have enjoyed sharing information on a local platform about a profession I am passionate about. Thank you for following my message.
Thank you to Nancy, my dental assistant of 26 years, who edited all my columns. Aside from correcting my sub-par spelling and punctuation, she also made many of the subjects I wrote about actually make sense.
And finally, thank you to Marc, founder/publisher of The Town Common, for giving me the opportunity to use this space for 19 years. I appreciate it very much.
Dr. St. Clair maintains a private dental practice in Rowley dedicated to health-centered family dentistry. He has a special interest in treating snoring, sleep apnea and TMJ problems. If there are certain topics you would like to see written about or questions you have, please email them to him at jpstclair@stclairdmd.com
MAKE ‘EM STICK
January 11, 2025
Happy New Year! So, how does it feel being back at work? Or, if you are retired, does today feel like any other day? For many people, the New Year is time for resolutions. Gym memberships go up and so do sales of healthier food. I don’t know about you, but I have trouble sustaining many of my “resolutions”. Change is difficult.
During the time I had off this past week, I re-read a book I read a few years ago. It is called “The Slight Edge” by Jeff Olson. One of the main points in this book is that change or improvement in our lives comes one day at a time. It is the small decisions that we make daily, that we often consider insignificant, which mold who we are.
In a recent column on New Year’s resolutions in the Wall Street Journal the author says, “Typically, though, people fail to stick to their annual goals because the resolutions are too demanding, vague or unrealistic.” One of the strategies recommended is to predict in advance what the roadblocks will be and how you will manage them. In addition to that, I have found that a daily reflection of all the day’s events and the changes I would make will make for a better tomorrow.
Changing routines is probably one of the hardest things to do. However, changing routines is probably one of the most important things to do. Striving for improvement in our lives by changing our routine usually improves the quality of life.
Going to the dentist is a routine. It is not part of your daily routine but it should be part of your overall routine for staying healthy. One of the biggest challenges I see in the practice of dentistry is changing people’s routines. Changing my own routines is tough enough; how does someone motivate someone else to change their routine? I think legendary coach John Wooden sums it up best when asked how he was so successful motivating his players for so many years. He said it was his ability to get his players to do what they didn’t want to do in order to get the results they wanted.
When someone goes to a dentist with a problem and has not seen a dentist for one, five, ten, or twenty years, it is easy to “fix” the immediate problem. The thing that is not easy to do, for any dentist, is to get those people to come back – to change their routine. While it is the dentist’s job to “fix” the problem, it is also their job to motivate people to see the bigger picture. Some people can be motivated to do those things they don’t necessarily want to do to achieve their goal (health), and others cannot.
Our priorities dictate our routines. Priorities need change just as much as routines. If our priorities include health, we will spend money on a gym membership or home fitness equipment, go to the doctor or dentist on a regular basis, and eat things that are healthy. If hypertension could be controlled by regular exercise and/or medication, doesn’t that beat an early heart attack? If periodontal (gum) disease, which doesn’t hurt and 75% of the population has some form of, could be controlled by regular visits to the dentist, doesn’t that beat losing your teeth?
Changing your routine to improve your quality of life is worth every penny you may spend on it. As Jeff Olson says in his book, “You can’t change the past. You can change the future. The right choices you make today, compounded over time, will take you higher and higher up the success curve of this real-time movie called ‘your life’.” Best wishes for positive change in 2025!
Dr. St. Clair maintains a private dental practice in Rowley dedicated to health-centered family dentistry. He has a special interest in treating snoring, sleep apnea and TMJ problems. If there are certain topics you would like to see written about or questions you have please email them to him at jpstclair@stclairdmd.com
21 SUGGESTIONS FOR SUCCESS IN 2025
January 6, 2025
At the end of each of the past 19 years, I have used this space to publish these 21 Suggestions for Success authored by H. Jackson Brown, Jr.
Cut this out and put it on the refrigerator. Read this list often and take these suggestions to heart.
- Marry the right person. This one decision will determine 90% of your happiness or misery.
- Work at something you enjoy and that’s worthy of your time and talent.
- Give people more than they expect and do it cheerfully.
- Become the most positive and enthusiastic person you know.
- Be forgiving of yourself and others.
- Be generous.
- Have a grateful heart.
- Persistence, persistence, persistence.
- Discipline yourself to save money on even the most modest salary.
- Treat everyone you meet like you want to be treated.
- Commit yourself to constant improvement.
- Commit yourself to quality.
- Understand that happiness is not based on possessions, power or prestige, but on relationships with people you love and respect.
- Be loyal.
- Be honest.
- Be a self-starter.
- Be decisive even if it means you’ll sometimes be wrong.
- Stop blaming others. Take responsibility for every area of your life.
- Be loyal and courageous. When you look back on your life, you’ll regret the things you didn’t do more than the ones you did.
- Take good care of those you love.
- Don’t do anything that wouldn’t make your Mom proud.
Best wishes for a happy, successful, and healthy 2025. Happy New Year!
Dr. St. Clair maintains a private dental practice in Rowley dedicated to health-centered family dentistry. He has a special interest in treating snoring, sleep apnea and TMJ problems. If there are certain topics you would like to see written about or questions you have please email them to him at jpstclair@stclairdmd.com
“IT’S JUST A CLEANING”
December 16, 2024
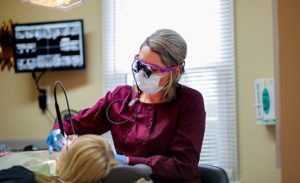 This is a phrase we hear far too frequently when patients call to cancel or change their dental hygiene appointments. When the patient is told that there are no open hygiene appointments for 4-6 months, the response is often, “Oh, that’s okay, it’s just a cleaning.” This lack of concern is only partly to blame on the patient; most of the accountability falls in the lap of the dental team.
This is a phrase we hear far too frequently when patients call to cancel or change their dental hygiene appointments. When the patient is told that there are no open hygiene appointments for 4-6 months, the response is often, “Oh, that’s okay, it’s just a cleaning.” This lack of concern is only partly to blame on the patient; most of the accountability falls in the lap of the dental team.
If you read this column with any frequency, I am sure you have seen me report that 75% of the population has some form of periodontal (gum) disease. I’m sure you have also read that periodontal disease has been linked to heart disease, stroke, pre-term, low birth-weight babies, diabetes, and possibly even some types of cancer. The problem is the dental team is not discussing this enough with their patients.
Here’s the way I see it: If a patient has made the decision to seek the services of a dental office, we must assume that the reason is based on wanting to improve and/or maintain their dental health. If that’s not the reason you go to the dentist, what is? Patients will often say during an exam, “Please don’t find anything.” Our response may be, “Well then, I better not look.” Assuming the reason for going to a dental office is to improve and/or maintain dental health as part of overall health, it is the obligation of the dental team to “find stuff” if it’s there, communicate that with the patient, and have a conversation about whether any steps should be taken.
For example, based on your level of periodontal health, there are different levels of frequency recommended for hygiene visits. The majority of patients should be seen every 6 months. Some are lucky enough to have yearly visits recommended to them. For others, every 3 or 4 months is recommended. This frequency is determined by your dental team to maintain your dental health. Regardless, if you put off your routine care by 1, 2 or even 6 months, that is a lot of time to have bacterial growth accumulate and put your body into a defensive mode due to increased inflammation. This brings me back to the reason you have chosen to be an active dental patient.
Remember, gum disease is not only bad because it makes your breath stink and your teeth fall out; it is bad for you systemically because of chronic inflammation. You may very well not notice an increase in inflammation, but your body does. There are measurable indicators of this.
If your goal is optimal health, routine maintenance is essential. I tell my team all the time that we must continue to educate the people who put their trust in us to maintain their dental health.
Depending on your car, there is a recommended maintenance schedule. If you ignore the recommended maintenance, only bad things can happen. You may be able to “stretch it out” a little, but must understand there are risks associated with that decision. If you knew how bad chronic inflammation really was for you, you would want to be seen more frequently than you are.
There are obviously valid reasons why patients need to change an appointment. Most dental offices understand that. It is the frequency, attitude (It’s just a cleaning), and lack of commitment that causes both disruption within the dental office and discontinuity of care.
Dr. St. Clair maintains a private dental practice in Rowley dedicated to health-centered family dentistry. He has a special interest in treating snoring, sleep apnea and TMJ problems. If there are certain topics you would like to see written about or questions you have please email them to him at jpstclair@stclairdmd.com
THE ORAL/SYSTEMIC LINK 3/3
December 2, 2024
 If you missed Part 1 and/or 2 of this series, you can find it at www.thetowncommon.com.
If you missed Part 1 and/or 2 of this series, you can find it at www.thetowncommon.com.
The past couple weeks have been about the growing evidence that links oral and systemic disease, and the need for more collaboration between dentists and physicians. All of this, of course, is in the best interest of the patient.
The body is a complex system – and everything is connected. The health status of an individual’s mouth can absolutely play a role in systemic health or disease. In addition to the need for dentists and MD’s to collaborate more on the oral/systemic connection, we also need to collaborate better about our patient’s sleep problems.
As part of a comprehensive approach to care, we screen for sleep issues with our patients. It amazes me how many people have issues with their sleep. It amazes me even more when I learn that many of these people have never even had a conversation with their doctor about sleep. Experts in sleep medicine agree that there is much room for improvement in this vital part of our health care.
Periodontal issues and sleep are just two areas where more information should be shared between dentists and physicians. We have to be open to the fact that everything is connected, and needs to be taken into consideration when we are trying to diagnose, monitor, or solve our patient’s problems.
I recently saw someone who has been a patient of mine for about 7 years. I noticed in the patient’s notes that bruxism/grinding had been discussed at most hygiene appointments in the past, due to the noticeable wear patterns on the patient’s teeth. There was also a note in the chart several times stating that the patient would never wear a dental appliance at night.
As I did my exam, I kept thinking to myself that there must be more to the story behind this patient’s dental issues. It happened to be around our lunch break, so I asked the patient if she had a few minutes for us to talk. She seemed interested in what I had to say. I photographed her teeth to compare them with photos taken 7 years ago. We talked for an hour.
Aside from learning that the patient was on (7) medications for the past SEVEN years and had never reported any of them to us, I also learned that the reason she was also resistant to wearing something to protect her teeth at night was because she had sleep issues. She felt there was no way she could handle the extra stuff in her mouth. I also learned that both of her parents are treated for sleep apnea.
So, here are some bullet highlights from the past 3 weeks:
- Periodontal (gum) disease is bad. Just because it doesn’t hurt doesn’t mean you don’t have a problem. If you care about your general health, you must take care of your mouth.
- Delaying care of dental problems always leads to more treatment and more cost.
- Don’t leave information out when discussing your health with your doctors. Everything is important.
- For better patient care, doctors and dentists should have more collaboration.
- Time is the most precious gift a health care provider can give their patients.
Dr. St. Clair maintains a private dental practice in Rowley dedicated to health-centered family dentistry. He has a special interest in treating snoring, sleep apnea and TMJ problems. If there are certain topics you would like to see written about or questions you have please email them to him at jpstclair@stclairdmd.com
THE ORAL/SYSTEMIC LINK 2/3
November 25, 2024
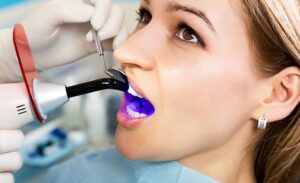 If you missed Part 1 of this series, you can find it at www.thetowncommon.com.
If you missed Part 1 of this series, you can find it at www.thetowncommon.com.
I ended last week with a statement that I have used numerous times before – just because it doesn’t hurt doesn’t mean there isn’t a problem. We keep learning more and more about the link between the mouth and the rest of the body. It is essential that dentists and physicians do a better job at co-managing patients, and learn more about the relationship between oral and systemic disease.
And if we’re being completely honest, there also needs to be a disruption in the insurance industry. Dr. Robin Davies (Byfield) said recently, “It just seems like common sense to me. If you had a chronic infection on your arm, wouldn’t you think it would affect your whole body? Why is it that the mouth is treated like it isn’t connected to everything else? A downfall of our healthcare system, for sure.”
It is clear, if you want to take better care of yourself, you need to take better care of your mouth. Familial history is very important. If you know of any family history of dental problems, you are at higher risk. Higher risk individuals need to be treated differently, and may need a more aggressive preventive protocol to help ward off progression of disease. In addition, an otherwise healthy person who presents with a sudden increase in gum inflammation should possibly be evaluated by their physician to rule out any systemic causes if there is not a simple explanation for the change.
Salivary biomarkers are among the tools being researched to help determine the particular disease path that a person is on. Although in their infancy, this precision approach to the prevention and treatment of periodontal disease accounts for variability in a person’s genes, environment, and lifestyle. Because it is more personalized to the individual, it results in more accurate treatment planning, as well as improved outcomes for the patient.
Considering the aging population, periodontal (gum) disease has the potential to become the most prevalent dental disease in the near future. It is more important than ever for dentists to take the time to develop and incorporate a comprehensive periodontal examination and treatment protocol for adults…..and to educate our patients on the importance and connection with rest of our bodies.
As with most diseases, delaying the treatment of periodontal disease until the advanced stages results in treatment that is more expensive, more complex, and less predictable. Most early to moderate stage disease can be treated in a general dental office if the inflammation is easy to control, the patient doesn’t have numerous systemic issues, and is determined to do their part at home. If all these things have been done without resolution, or if the periodontal disease is more severe, it may be in the patient’s best interest to be referred to a like-minded periodontist. A periodontist is a specialist who treats disease of the gums and bone that support the teeth.
When half of the US population is still affected with periodontal disease, despite decades of research and treatments, something is still missing. That missing key is a more collaborative approach involving, dentists, periodontists and physicians.
….and remember, just because it doesn’t hurt doesn’t mean there isn’t a problem. To be continued.
Dr. St. Clair maintains a private dental practice in Rowley dedicated to health-centered family dentistry. He has a special interest in treating snoring, sleep apnea and TMJ problems. If there are certain topics you would like to see written about or questions you have please email them to him at jpstclair@stclairdmd.com
THE ORAL/SYSTEMIC LINK 1/3
November 18, 2024
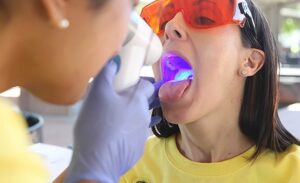 The connection between oral health and systemic health is well-established and ever-evolving. One thing we know for certain; we are living longer, but with more chronic diseases and medication than ever before.
The connection between oral health and systemic health is well-established and ever-evolving. One thing we know for certain; we are living longer, but with more chronic diseases and medication than ever before.
The latest statistics are alarming. Forty-seven percent of US adults who are age 30 or older – an estimated 64.7 million Americans – have either mild gum disease (8.7%), moderate gum disease (30%) or severe gum disease (8.5%). As the population ages, the prevalence rises with 70% of individuals over the age of 65 exhibiting some level of gum disease. And, since we are on statistics, by 2030, it is estimated that the number of people over 70 years of age will have doubled from 35 million to 71 million.
As we age, our risk of developing disease increases. Interestingly, there is also a direct correlation between the regions of the US with the greatest concentration of gum disease, and those that have a high incidence of cardiovascular disease and diabetes. Although a direct cause-and-effect link is still in the process of being established between gum disease (periodontitis) and other systemic diseases, inflammation is often a common denominator. And it is always important to remember that the mouth is the gateway to the rest of the body.
We used to think that if people didn’t brush their teeth well, or didn’t visit a dentist often, they would automatically get gum disease. However, there are patients who have poor home care who never develop gum disease, and there are also patients who have great home care, visit a dentist regularly, and continue to experience breakdown from gum disease – albeit at a slower rate than they would if they had poor habits.
We now know that managing gum disease and other chronic inflammatory diseases like cardiovascular disease, diabetes, respiratory disease and arthritis are more patient specific based on an individual’s “inflammatory mediators”. These are molecules released by immune cells and are largely responsible for individual responses to disease susceptibility and progression. This is why probiotics are likely to play a significant role in treatment of chronic inflammation in the future.
As we wait for research development for different ways to combat chronic inflammation, it is without dispute that people should do all they can to minimize inflammation in the mouth. The mouth is very accessible and with proper training, coaching and monitoring, a healthy mouth is better for your whole body.
Although some may say that the associations between gum and systemic diseases are statistical by nature, not causal, the data is fairly strong that there is a link between gum disease and cardiovascular disease – such as heart infarction and stroke. This supports diagnosing and treating oral infections, including lifelong professional maintenance and good home care.
Just because it doesn’t hurt doesn’t mean there isn’t a problem. More next week.
Dr. St. Clair maintains a private dental practice in Rowley dedicated to health-centered family dentistry. He has a special interest in treating snoring, sleep apnea and TMJ problems. If there are certain topics you would like to see written about or questions you have please email them to him at jpstclair@stclairdmd.com
UNDERSTANDING YOUR BENFITS
November 12, 2024
 I think it is safe to say that our healthcare system has some flaws. Wouldn’t it be nice to have a healthcare system that realized that everything in the body is connected? Unfortunately, there are no reasonable solutions for this in the near future. Therefore, it is important for you to take your health into your own hands and plan appropriately.
I think it is safe to say that our healthcare system has some flaws. Wouldn’t it be nice to have a healthcare system that realized that everything in the body is connected? Unfortunately, there are no reasonable solutions for this in the near future. Therefore, it is important for you to take your health into your own hands and plan appropriately.
Patients will sometimes balk at treatment not covered by their dental insurance. Dentists will often hear, “Just do what my insurance covers. I don’t want anything extra.” In fact, a recent ADA poll showed that a lack of dental insurance was the #1 reason most patients gave for not visiting a dentist. Here are some frequent questions patients often ask about dental insurance.
Why doesn’t my insurance cover all of the costs for my dental treatment?
Dental insurance isn’t really insurance (defined as a payment to cover the cost of a loss) at all. It is a monetary benefit, typically provided by an employer, to help their employees pay for routine dental treatment. “Dental Insurance” is only designed to cover a portion of the total cost.
But my plan says that my exams and other procedures are covered at 100%.
That 100 percent is usually what the insurance carrier allows as payment towards a procedure, not what your dentist may actually charge. Dentist’s fees are usually a reflection of the level and quality of care in a particular office. Some cost more, some cost less, depending on the costs of running their office, how much they pay their staff, the materials they use, etc. An employer usually selects a plan with a list of payments that corresponds to its desired premium cost per month. Therefore, there usually will be a portion not covered by your benefit plan.
If I always have to pay out-of-pocket, what good is my insurance?
Look at medical insurance. Many people have been forced into high deductible plans ($2000 or more). Most dental plan deductibles are $50. While dental insurance is far from ideal, any amount that reduces your out-of-pocket expense helps.
Why is there an annual maximum on what my plan will pay?
Although most maximum amounts have not changed in 30+ years, a maximum limit is your insurance carrier’s way of controlling payments. Dental plans are different from medical plans, in that dentistry is needed frequently. Medical emergencies are rare. It is your dentist’s responsibility to recommend treatment based on diagnosis and treatment planning of what is appropriate for your dental health, not necessarily what your dental plan covers.
If my insurance won’t pay for this treatment, why should I have it done?
It is a mistake to let your benefits be your sole consideration when you make decisions about dental treatment. People who have lost their teeth often say that they would pay any amount of money to get them back. Your smile, facial attractiveness, ability to chew and enjoy food, and general sense of well-being are dependent on your teeth.
Other than complaining to your dental insurance company or your Employee Benefits Coordinator, your best defense is to budget for dental care. First, find a provider based on a personal fit for you. That is the single most important thing you can do. If that office can’t work with you financially then I would find another office.
Dr. St. Clair maintains a private dental practice in Rowley dedicated to health-centered family dentistry. He has a special interest in treating snoring, sleep apnea and TMJ problems. If there are certain topics you would like to see written about or questions you have please email them to him at jpstclair@stclairdmd.com
ADULT SLEEP
November 4, 2024
 Last week was teenager sleep patterns and issues. This week we start a conversation about how our sleep needs and potential issues as adults.
Last week was teenager sleep patterns and issues. This week we start a conversation about how our sleep needs and potential issues as adults.
We all do better when we get good quality sleep. For some people though, sleep quality is consistently poor. There are many folks out there who “get by”, but are not functioning at full capacity due to poor sleep. Many of them think they sleep fine, but they don’t.
Insomnia, difficulty with falling asleep or staying asleep for more than 3 nights a week, is the most common sleep disorder. Sleep “hygiene” improvement, along with cognitive behavior therapy, is the first course of action to treat this problem.
There are many reasons for poor quality sleep. Some are easier to control than others. Everything from a poor mattress, poor pillow, sleep position, medical issues, diet, alcohol consumption, and work schedule can have an impact on the quality of sleep that we get. Although some people can notice subtle changes in sleep quality, many others do not realize that some of the issues they have routinely can be caused from poor sleep quality.
Sleep plays a vital role in good health and well-being throughout our lives. The way you feel while you’re awake depends in part on what happens while you’re sleeping.
Sleep helps your brain work properly. Studies show that a good night’s sleep improves learning. Studies also show that sleep deficiency may cause you to have trouble making decisions, solving problems, controlling your emotions and behavior, and coping with change.
Sleep plays an important role in your physical health. For example, sleep is involved in healing and repair of your heart and blood vessels. Ongoing sleep deficiency is linked to an increased risk of heart disease, kidney disease, high blood pressure, diabetes, stroke, sexual dysfunction, ADHD, obesity and depression.
Sleep issues can affect the young, the old and everyone in between. The many changes that take place in our bodies as we age can increase the risk of sleep disorders.
Sleep apnea is another common sleep disorder. It is a serious, potentially life-threatening sleep disorder that affects approximately 18 million Americans. It comes from the Greek meaning of apnea which means “want of breath”. People with sleep apnea have episodes in which they stop breathing for 10 seconds or more during sleep.
People with sleep apnea do not remember these episodes during the night, unless they awake to a gasp. Some of the potential problems may include morning headaches, excessive daytime sleepiness, irritability and impaired mental or emotional functioning, excessive snoring, choking/gasping during sleep, insomnia, or awakening with a dry mouth or throat.
Some simple questions to ask yourself are: Have you been told that you snore?
Do you often feel tired, fatigued, or sleepy during the daytime?
Has anyone ever told you that you stop breathing while you were asleep – or- Have you ever woken yourself up with a gasp?
Do you take more than one medication to control high blood pressure?
Are you a mouth breather? Do you need to use the bathroom multiple times at night?
Is your body mass index greater than 28?
If you answered yes to more than two of these questions, or if there is anything else in this column that makes you believe you may not be getting the quality of sleep you would like, please discuss these with your physician.
Dr. St. Clair maintains a private dental practice in Rowley dedicated to health-centered family dentistry. He has a special interest in treating snoring, sleep apnea and TMJ problems. If there are certain topics you would like to see written about or questions you have please email them to him at jpstclair@stclairdmd.com
TEEN SLEEP
October 28, 2024
 When we were all young children, most of us got plenty of sleep, and for that matter, we didn’t think much of it. Our parents told us it was time for bed and we went to bed. We slept until the morning at which time we were woken by our parent’s gentle touch.
When we were all young children, most of us got plenty of sleep, and for that matter, we didn’t think much of it. Our parents told us it was time for bed and we went to bed. We slept until the morning at which time we were woken by our parent’s gentle touch.
As we progressed into our teenage years, our responsibilities increased. This typically led to staying up later and getting up earlier to be able to keep up with these added responsibilities. Today, it seems that getting enough good sleep is even more of a challenge for our teenagers.
One of the contributing factors of this teen sleep crisis is that parents are not as strict with setting rules for sleep as they were when their children were younger. It is not uncommon for teenagers to say to their parents they are going up to their room to do homework and then go to bed.
I recently asked my daughter (a freshman in college) what time she generally “packed it in” and settled down to fall asleep. She told me that after she finishes her homework she will lie in bed and watch something on her laptop until she feels sleepy. This trend is an antithesis to good sleep and one that must be discussed with every teenager by their parents.
Rules about electronics, which include cell phones, computers, games and the television, are especially crucial. In a study done by the National Sleep Foundation, it was determined that teens who have electronic devices on prior to going to sleep, get an average of 30 minutes less sleep. There are other studies that show that the quality of sleep is also greatly affected by this same practice.
Another, more obvious rule that parents must enforce, is the consumption of caffeine at night. Any form of caffeine should not be consumed after dinner. Studies indicate that caffeine in the system accounts for almost a full hour less of quality sleep. We, and our teenagers, cannot afford this deprivation of sleep.
We all start our days at different times. For the teenager, getting up to get ready for school can start pretty early. There is a “start school later” movement that recently received a powerful boost from the Centers of Disease Control and Prevention (CDC). The CDC report showed that teenage students have biologically different sleep patterns and needs than in other stages of life. Starting school a half hour later or more provides the teenager the opportunity to consistently get a better night’s rest.
For the teenager, managing homework and extracurricular activities is also definitely a barrier to sufficient sleep. We as parents must discuss this with our children to provide support with time management. If necessary, we must also not be afraid to discuss this with teachers and coaches if our teenager is struggling to get everything accomplished, thus affecting their sleep patterns.
As adults, many of us have our own routines that could use a revision to get more quality sleep. That is a subject for another time. As parents, it is our responsibility to guide our children to practice good habits. Discussing and enforcing better sleep habits is a gift that keeps on giving.
Dr. St. Clair maintains a private dental practice in Rowley dedicated to health-centered family dentistry. He has a special interest in treating snoring, sleep apnea and TMJ problems. If there are certain topics you would like to see written about or questions you have please email them to him at jpstclair@stclairdmd.com